Measurement-Based Care: A Data-Driven Approach to Better Mental Health
Mental health care is changing, and one of the most significant developments in recent years has been Measurement-Based Care (MBC).
This evidence-based approach improves standard mental health treatment by incorporating real-time data collection and feedback into therapeutic decision-making.
By rigorously tracking patient progress, MBC improves treatment results, patient involvement, and provider efficacy.
Despite its proven advantages, MBC is underutilized. Many clinicians have yet to see its potential, and patients are unaware of how data-driven treatment might enhance their outcomes.
What is Measurement-Based Care?
Measurement-Based Care (MBC) is a structured method of providing treatment involving regular, standardized evaluations of a patient’s symptoms, functioning, and treatment response.
These assessments, which are commonly conducted using empirically validated self-report questionnaires or clinician-rated tools, assist therapists in making data-driven decisions and adjusting treatment programs accordingly.
Unlike traditional mental health care, where changes are frequently based on subjective assessments, MBC provides objective data to inform clinical decisions. Patients perform routine assessments with standardized tools and physicians analyze the outcomes to verify treatment is working properly.
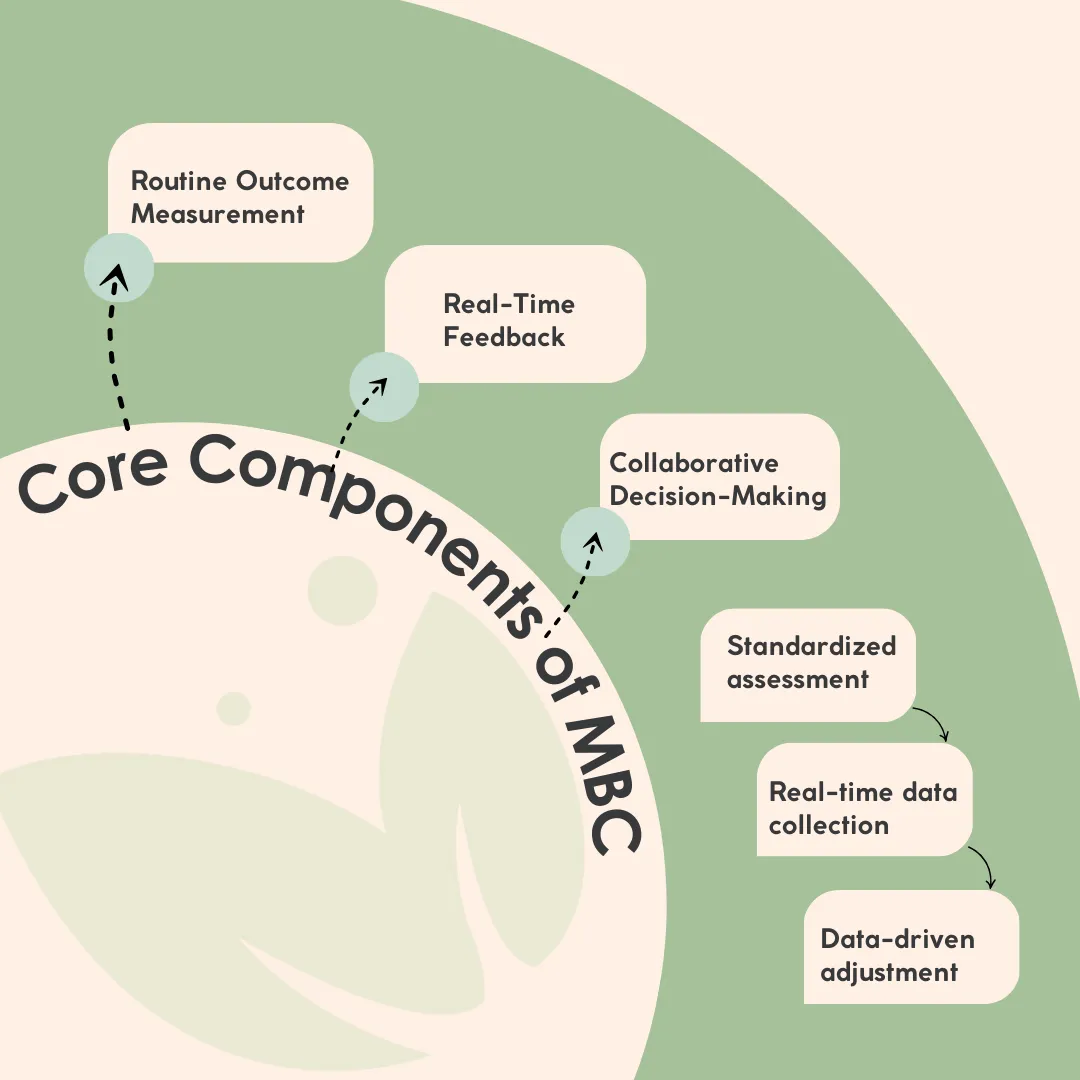
Core Components of MBC:
- Routine Outcome Measurement – Patients complete standardized assessments at regular intervals such as
- Patient Health Questionnaire (PHQ-9) for depression
- Generalized Anxiety Disorder Scale (GAD-7)
- Clinician-Administered PTSD Scale (CAPS-5)
- And more
- Real-Time Feedback – Clinicians analyze data to monitor progress and adjust treatment strategies
- Electronic health records and digital platforms streamline data collection
- Mobile apps allow patients to submit self-reports remotely
- Wearable devices can track physiological responses linked to mental well-being
- Collaborative Decision-Making- Patients and providers use objective data to inform care decisions
- Clinicians analyze trends over time to measure treatment effectiveness
- Adjustments to therapy or medication are made based on quantifiable evidence, not just clinical judgement
- Patient and providers collaborate on treatment modifications, improving engagement and adherence
Standardized assessment → Real-time data collection → Data-driven adjustment
Why Measurement-Based Care Matters: The Evidence
Scientific research has shown that MBC considerably improves mental health outcomes when compared to standard symptom-based methods. Key advantages include:
- Improved Patient Outcomes: Patients who receive MBC have lower symptom levels and higher treatment adherence compared to those in standard care
- Enhanced Clinical Effectiveness: MBC offers physicians objective data, reducing their reliance on subjective impressions
- Increased Patient Engagement: Patients who actively track their symptoms report feeling more empowered and involved in their care, which leads to higher levels of satisfaction and adherence
- Early detection of treatment gaps: MBC identifies non-responders early, allowing for prompt intervention and treatment changes
Despite these benefits, A 2023 survey found that only 46% of behavioral health care practitioners use MBC with at least half of their patients.
Why isn’t MBC more widespread?

Overcoming Barriers to MBC Implementation
While MBC is a game-changer, there are still hurdles that prevent widespread adoption
- Time constraints
- Many physicians are concerned that regular assessments will add work to a busy schedule.
- Solution: Automated digital solutions help speed up the process by incorporating evaluations directly into existing workflows.
- Lack of Training
- Some mental health providers are unfamiliar with the data analytic approaches required for MBC.
- Solution: Training programs and analytics can improve patient data interpretation efficiency.
- Patient Resistance
- Some people are overwhelmed by frequent assessments and see them as impersonal.
- Solution: Educate patients on how self-reported data might help them become more engaged.
- Technology Gaps
- Smaller offices may have limited access to electronic health records systems and data tracking platforms.
- Solution: Affordable smartphone apps and cloud-based technologies are developing as non-hospital options. Alternatively, measures can be completed with pen and paper

Real-World Applications of Measurement-Based Care – A Case Study
A major community mental health clinic used MBC to follow depression and anxiety with the PHQ-9 and GAD-7.
Over 6 months, individuals who received MBC-guided care experienced a 30% reduction in symptoms compared to those receiving traditional treatment.
The clinic also observed increased patient retention rates and more effective clinical decision-making.
The Future of Measurement-Based Care
Over the next decade, MBC is projected to become an amazing tool in mental health therapy. Future innovations include:
- Cultural Adaptation of MBC: Ensuring that assessments and interventions are customized to varied communities
- Integration with Value-Based Care Models: Healthcare systems will provide financial incentives for outcome-driven mental health care.
With an increased emphasis on evidence based practice, MBC has the potential to transform how mental health professionals provide care.
It takes an organized, data driven approach to ensuring therapies are effective, flexible and patient-centred.
By incorporating objective data into mental health treatment, MBC improves results, increases patient engagement, and reduces guesswork in care decisions.
The future of mental health care is data-driven, and MBC is paving the way.
Further Reading
- A tipping point for measurement-based care. Psychiatric Services (https://doi.org/10.1176/appi.ps.201500439)
- Using measurement-based care to enhance any treatment (https://doi.org/10.1016/j.cbpra.2014.01.010)
- Implementing routine outcome monitoring in clinical practice: Benefits, challenges, and solutions (https://doi.org/10.1080/10503307.2013.817696)
- Evidence-based care and measurement-based care: Complementary or contradictory approaches to improving mental health care? (https://doi.org/10.1007/s10488-018-0893-7)
- Self-Assess Your Own Mental Health
Disclaimer:
This information is for educational purposes only and does not constitute professional medical advice. Always consult a healthcare professional before incorporating any new therapy into your practice.
Do you want to see all the updates?
👉 Follow us on Instagram and Facebook and never miss a thing!